An insight into the huge odds that face some of the world's tiniest newborns.
We met Polite and Walter in the Kangaroo Care ward of a district hospital in Zimbabwe; a specialist ward that teaches parents essential skin-to-skin contact to bond with their babies, keep them warm and support breastfeeding amongst other benefits. Their tiny baby Unity was wrapped in blankets on the bed behind them, deep in sleep.
Unity is the young couple’s second child. She was born eight weeks premature at a Severely-Low Birth Weight less than a third of what a healthy baby is expected to weigh. When we met her, she was one-month-old and weighed only 1.45kg. At this age, a healthy baby should weigh more than four kilos.

Underlying the rising neonatal deaths, Zimbabwe has a very high rate of preterm births. “We’re ranked number four in the world,” says Jennifer Barak, UNICEF Zimbabwe’s Health Manager. At many of the hospitals Jennifer visits, newborns are dying from preventable causes due to poor quality of care linked to human resource shortages, unavailability of consistent water and electricity supply and general limited resources that hospitals receive.
Thankfully, Unity is now gaining weight and will soon be discharged. “Only 50 grams to go,” says her dad, Walter happily. New mum Tendai and her first born son, Vision, are also in the ward. Vision was born at 29 weeks and was even smaller than Unity. He hasn’t been gaining weight and nurses are worried.
The World Health Organisation recommends premature babies stay in health care facilities until they weigh at least 2.5kg. Here however, at the small district hospital, there are not enough beds to keep the babies this long.
"We lose so many [babies] during this period."
Unity will be leaving the hospital while she’s still classified as low-weight and at-risk of ongoing complications.
“Many newborns are dying in communities but these deaths go unreported,” says Jennifer. Once women return home, they have extremely limited access to health services because of the long distances they need to travel to similarly under-resourced rural healthcare clinics.
These challenges mean that women and their babies are being sent back into sometimes extremely remote communities too soon, and Zimbabwe’s families are feeling the most brutal impact.

“We lose so many [babies] during this period,” shares Jennifer. “There hasn’t been the decline in newborn mortality we’d want to see… We want strong health systems that ensure health facilities are equipped with the right skills equipment to be able to respond and ensure that we’re not missing opportunities to save lives.”
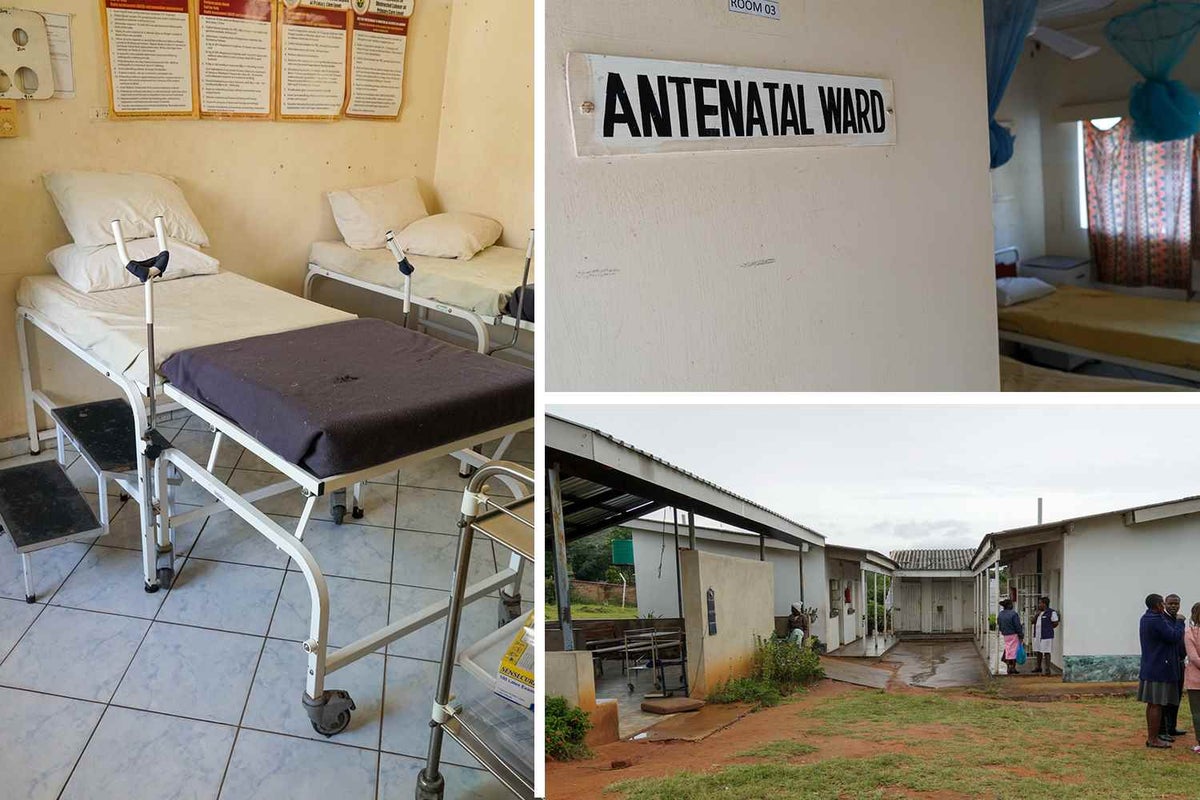
The situation is even more dire as you move to the rural health clinics, designed to lighten the load of referrals to the larger district hospitals. A Nursing Environment Technician at one of these rural clinics, Judith, explains that at times women have been forced to give birth on the floor. At many of these rural clinics, the same room is used as a perinatal, antenatal and labour ward.
While the situation in Zimbabwe is challenging, UNICEF is working with the government to fill some of the most devastating gaps in the health care sector that are directly contributing to the preventable deaths of women and their newborn babies.
One UNICEF-led initiative making huge progress in rural areas is the Village Health Worker (VHW) program. These village-nominated health workers play a vital role; following up on the health of all newborns and children under the age of five in some of Zimbabwe’s remote communities.
This work is especially important for low-weight babies like Unity and Vision; VHW’s can recognise danger signs and timely refer and accompany caregivers to local medical centres so that the baby can start receiving immediate medical care.

With the help of donors, we’ve made huge strides in development; helping to reduce maternal mortality by almost 30% in the last five years. Newborns are dying in increasing numbers however and UNICEF is working with the local governments to learn more about why this is happening.
“This year we’re looking at strengthening perinatal death audits to understand better why these babies are dying and furthermore promote the lessons learned to improve care and save lives the next time,” says UNICEF Zimbabwe Health Manager, Jennifer.

With your help we’ve been able to provide essential services to those who need them most. But newborns are still dying from preventable causes and we need your help now more than ever to strengthen the healthcare services available in Zimbabwe to save the lives of mothers and their babies.
Please, donate now and help newborns survive and thrive, even against some of the most incredible odds in the world.
Related articles
Stay up-to-date on UNICEF's work in Australia and around the world
















