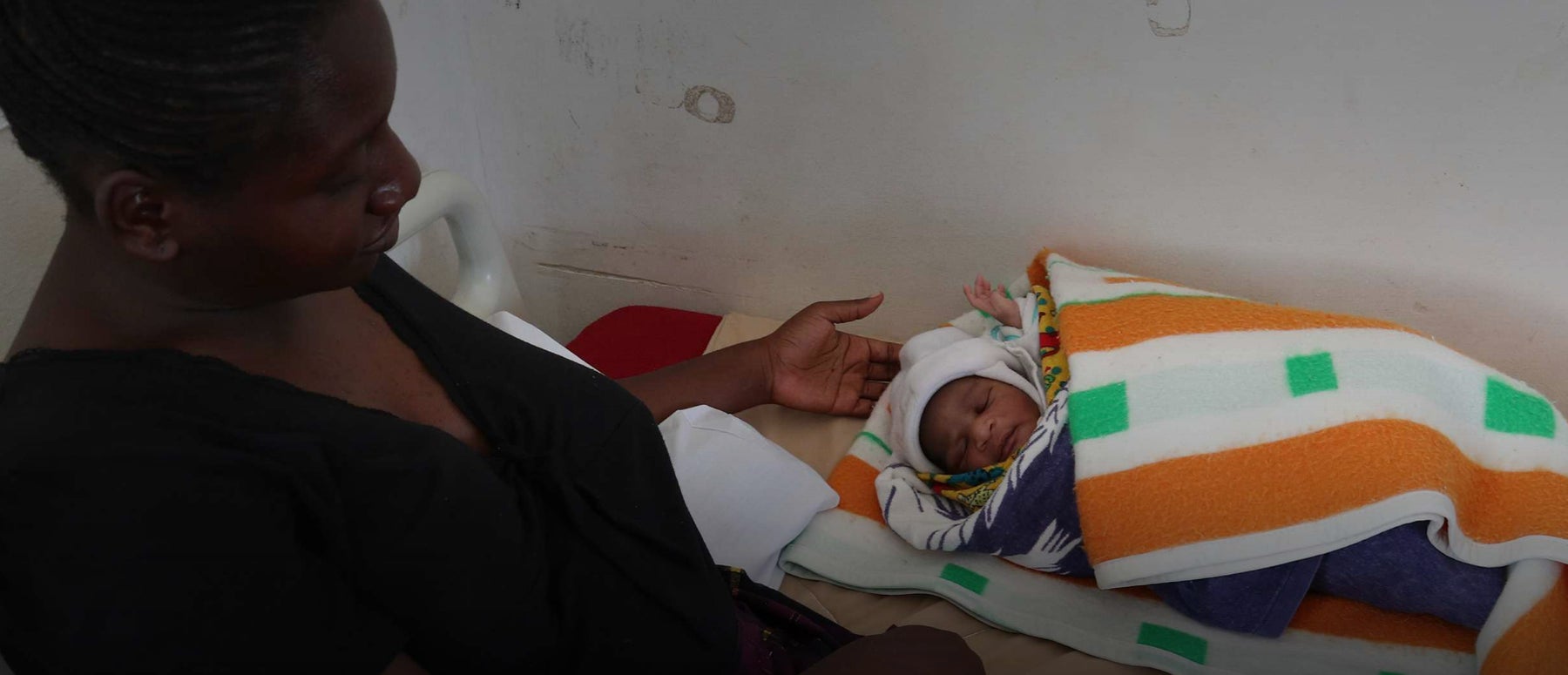
Being pregnant in Zimbabwe is a dangerous experience.
UNICEF International Programs Coordinator and Wollongong resident, Bethany Stirling, has just returned from visiting our child survival programs in Zimbabwe.
Maternal mortality rates are amongst the worst in the world, and a staggering 55 times higher than in Australia. Women and babies are dying in childbirth – and they shouldn’t be.
In Guruve district, many families live in poverty and the upcoming drought season means food and water will soon become scarce. Few families here can afford transport, so most patients walk to healthcare.
This means women must choose between giving birth at home without medical assistance or walking for hours to reach healthcare once they know it’s time.

The local health centres are very basic. At the Matsvitsi Health Clinic thin mattresses cover steel beds, and there’s not much privacy or space.
Thankfully they now have solar power so they can assist mothers who give birth at night.

Despite this the staff here are so proud of the support they can provide to mothers, working hard to make the most of the facilities and supplies they have.
Many of the local-level health clinics and district hospitals are under-resourced and without doctors skilled in emergency obstetric care. If complications arise pregnant mothers are often far from help and need to be referred across the country to larger hospitals – an expensive and dangerous journey, which means some patients don’t reach healthcare in time.
To help change this, UNICEF is working to improve the level of healthcare at remote health clinics and district-level hospitals by running a mentorship program. Doctors in the districts are trained and supported by mentors from the larger hospitals in emergency obstetric and newborn care.
This means mothers from remote areas can receive the care they urgently need straight away, instead of travelling hours to larger hospitals.
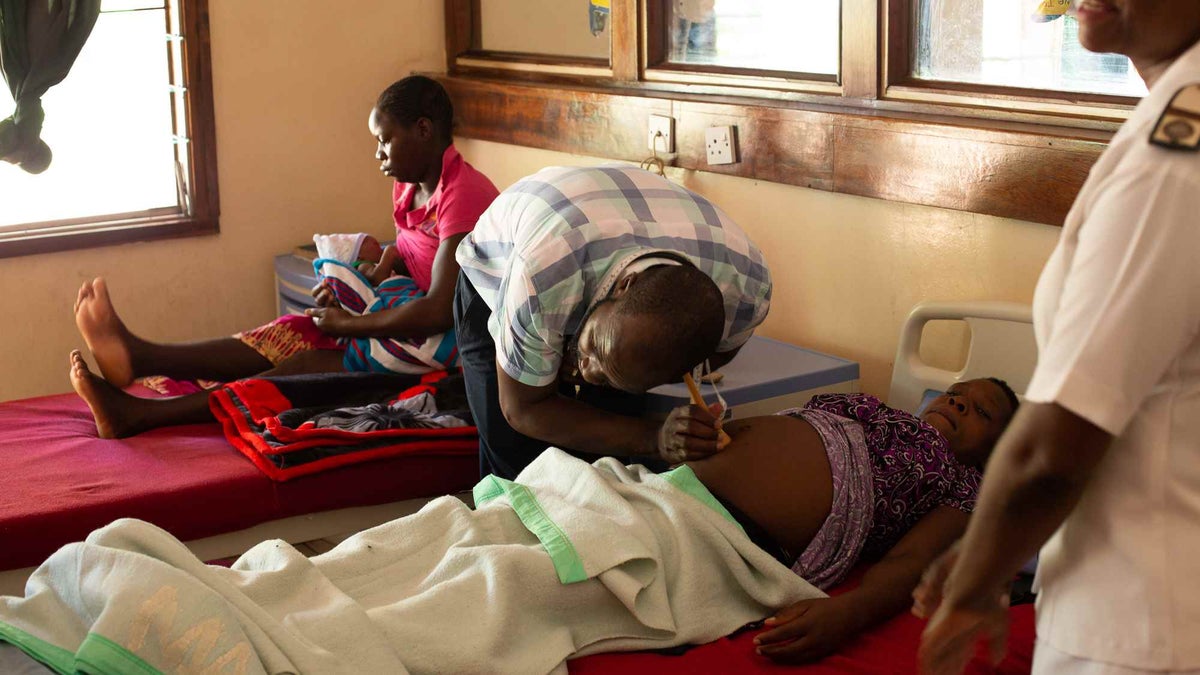
One patient my team met was Rudo from Binga, a remote district in northern Zimbabwe close to the border with Zambia.
When my team met her, she had been in labour for 16 hours. Her blood pressure was high, her unborn baby was facing in the wrong direction for delivery and the baby’s heartbeat was weak.
The physician on the scene, Doctor Goronga, had never faced such a complicated delivery.
In moments like this, time is of the essence and medical expertise is critical if Rudo and her child are to survive. Thanks to UNICEF’s mentoring program, an experienced doctor was available to mentor Doctor Goronga through the difficult childbirth, helping him perform an emergency caesarean.
“We were able to deliver a healthy baby for Rudo,” Doctor Goronga happily told us.
Rudo and her beautiful baby girl were lucky, and they are both now doing well.
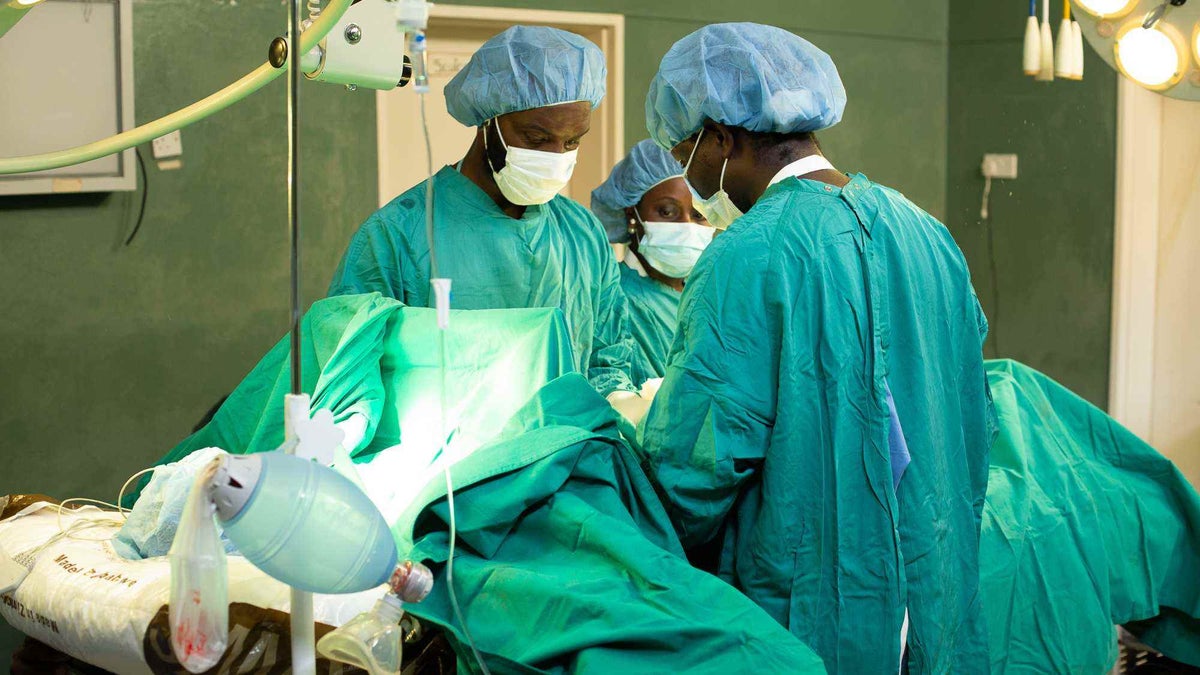
The benefit of the program is overtime medical staff, like Doctor Goronga, gain the skills and experience they need to perform these operations solo – and then help train their colleagues.
Since the start of the program in 2017, Binga District Hospital has not recorded one single death during deliveries.
Doctors at the major hospitals have also noticed a decline in referrals, with district-level doctors able to manage more cases on their own.
On my visit I met two mentees who had operated a caesarean section on a mother just the week before. Before closing the incision, they checked the other side of the uterus, as they were taught by their mentors.
They found a rupture that they were able to repair before closing the incision.
The mother would have bled to death if they didn’t check.

Another way to improve maternal mortality and child survival rates in Zimbabwe is through supporting village health workers.
Village health workers go door-to-door sharing advice with expectant mothers on the best ways to look after themselves and to take care of their newborns, such as the importance of breastfeeding.
They also promote the practice of giving birth at a health centre rather than risking staying at home. Many district hospitals and some clinics have also been able to build waiting homes for women to stay at in advance of giving birth so they are close to medical care when the time comes.
“Behaviour change is not instant,” explains Bugalo, who been a health worker for over 11 years.
“I persistently convey health education to the women, and now mothers are more aware of health issues.”
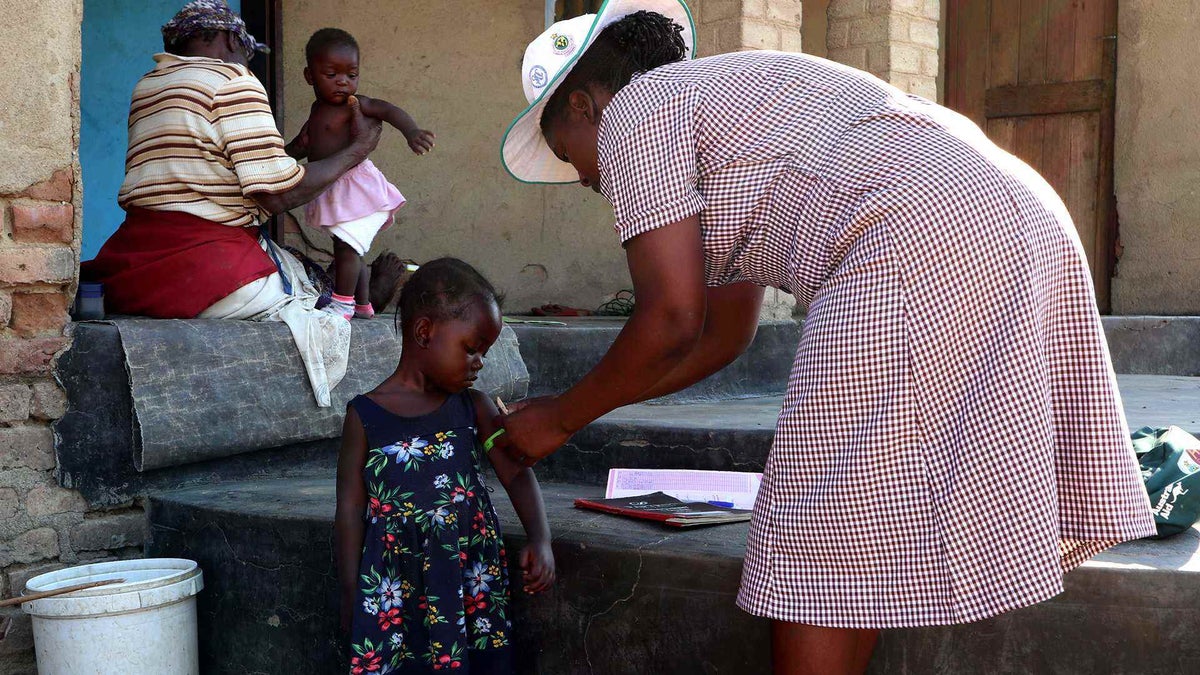
UNICEF helps to deliver supplies for health workers such as utility kits that include life-saving tools like scales, thermometers, torches and batteries. We also provide bicycles to make it easier for the health workers to travel long distances to meet their patients.
With support from DFAT’s Australian NGO Cooperation Program, UNICEF’s child survival program has been trialled in five districts in Zimbabwe. Following the success of the program, UNICEF is now working to expand the programs in 15 more districts as soon as possible, so more mothers and their newborns can be saved.

Related articles
Stay up-to-date on UNICEF's work in Australia and around the world